What is Cognitive Behavioural Therapy? And How Does it Actually Work?
By Alex Aslan | Registered Psychologist, Sydney CBD
Most people have heard of CBT. Fewer people actually know what happens in the room.
If you've been thinking about therapy and keep seeing "cognitive behavioural therapy" mentioned by your GP, on a mental health plan, or in a late-night Google search, this article will give you a clear, honest picture of what it is, what a session actually involves, and whether it might be the right fit for what you're dealing with.
I'm a registered clinical psychologist based in Sydney CBD, and CBT is one of the primary frameworks I use with clients. Here's what I'd tell you if you asked me to explain it properly.
The core concept underlying CBT
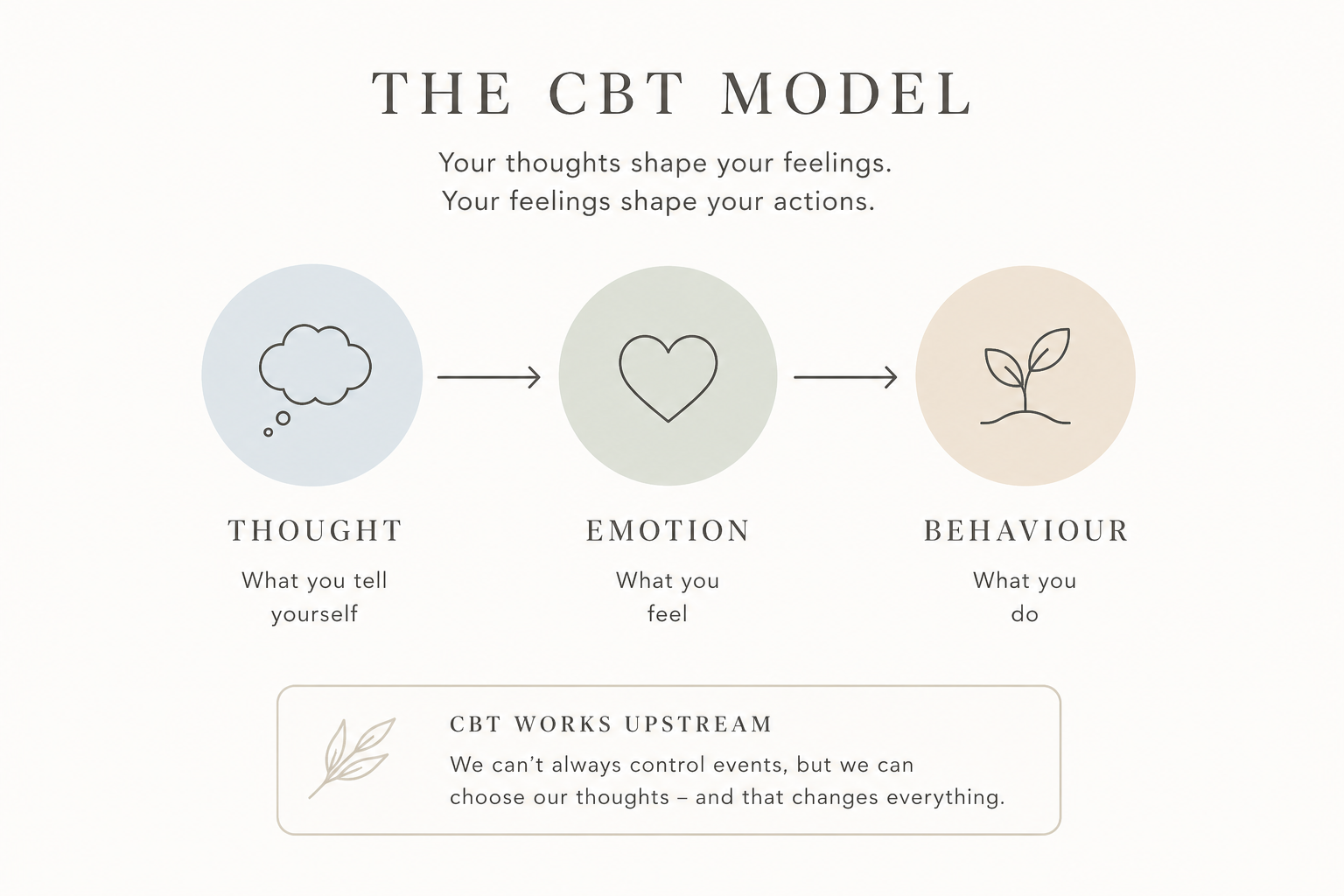
Cognitive behavioural therapy is built on a deceptively simple observation: the way you think about a situation directly shapes how you feel about it — and how you feel shapes what you do.
The chain of thought, emotion, behaviour is the engine of CBT.
Here's an example. Two people receive the same critical feedback from their manager. One thinks, "They've noticed something I can improve." The other thinks, "I'm failing and they're building a case to let me go." Same event. Completely different emotional experiences, and then completely different behaviours: one person acts on the feedback, the other spends three nights unable to sleep.
CBT works upstream at the level of interpretation and asks: is this thought accurate? Is it helpful? Is there another way of looking at this that is more realistic and less corrosive?
Common CBT misconceptions
It's not "just think positive." CBT doesn't ask you to replace negative thoughts with cheery affirmations. It asks you to examine your thoughts like a scientist — looking for evidence, testing assumptions, and landing on something more accurate. Sometimes the realistic thought is still difficult. But difficult-and-accurate is far more workable than difficult-and-distorted.
It's not surface-level. A well-delivered course of CBT uncovers the underlying beliefs driving your thinking patterns, often beliefs about yourself or the world that have been operating quietly for years. That's where lasting change happens.
It's not a quick fix. CBT requires engagement between sessions. The payoff is that the skills become yours permanently, you don't remain dependent on a therapist to manage your mental health.
What is the evidence for CBT?
CBT is one of the most rigorously studied psychological treatments in existence. It's recommended as a first-line treatment in Australian clinical guidelines for anxiety, depression, OCD, PTSD, and insomnia, among others.
The research consistently shows that CBT produces outcomes comparable to medication for mild to moderate depression and anxiety and with lower relapse rates, because you've built skills rather than just managed symptoms. The benefits also tend to hold long after treatment ends.
What happens in a CBT session?
CBT sessions are structured, which distinguishes them from more free-flowing therapy conversations. A typical session involves:
Check-in: A brief review of the week, mood, and any significant events since the last session.
Homework review: CBT involves work between sessions — thought records, behavioural experiments, activity logs. We review what came up.
Core work: Identifying and challenging a thought pattern, working through avoidance, processing a difficult experience, or building a specific skill.
Summary and next steps: Consolidating what came up and agreeing on what to practise before the next session.
Most people find the structured format takes some adjustment, then come to appreciate it. There’s a sense of direction, and you can see what you're working toward.
What are the core techniques in CBT?
CBT draws on a range of evidence-based methods. The most common include:
Thought records — catching automatic thoughts, examining the evidence for and against them, and generating a more balanced response. The backbone of CBT for anxiety and depression.
Behavioural activation — used primarily in depression. When people are low, they tend to withdraw and stop doing things they used to enjoy, which deepens the depression. Behavioural activation rebuilds engagement systematically, because action tends to precede motivation rather than follow it.
Exposure — the cornerstone of anxiety treatment. Avoidance keeps anxiety alive. Exposure involves gradually facing feared situations in a controlled, collaborative way, allowing anxiety to decrease naturally and confidence to build.
Cognitive restructuring — identifying cognitive distortions (catastrophising, black-and-white thinking, mind reading) and learning to generate more accurate, flexible alternatives.
Behavioural experiments — testing beliefs in real life rather than just talking about them in session.
How many sessions does CBT take?
This depends heavily on the presenting problem:
Specific phobias: as few as 4–6 sessions
Anxiety disorders and depression: typically 12–20 sessions
OCD: often 20+ sessions
Trauma and PTSD: typically 12–20 sessions with a trauma-focused approach
In Australia, a Mental Health Treatment Plan from your GP gives you access to Medicare rebates for a set number of psychological sessions per calendar year. It's worth organising this before you book.
What is the difference between CBT and ACT?
You may have also heard of Acceptance and Commitment Therapy (ACT), sometimes described as a newer wave of CBT.
Traditional CBT focuses on changing the content of unhelpful thoughts — questioning them, testing them, replacing them with more accurate alternatives.
ACT takes a different angle. Rather than changing your thoughts, it focuses on changing your relationship to them. The idea is that trying to suppress or argue with difficult thoughts often makes them stronger. Instead, ACT teaches you to observe thoughts with some distance, accept difficult emotions without being controlled by them, and commit to action aligned with your values.
In practice, most good therapists draw on both, matching the approach to the person and the problem.
Is CBT right for you?
CBT tends to work best for people who are dealing with a specific, identifiable problem; who are willing to engage actively between sessions; and who want to understand the mechanisms driving their difficulties — not just feel better in the room.
It's also worth nothing that CBT isn't for everyone. Some people find the structured approach too present-focused. Others find the homework demanding during periods of low motivation. A good therapist will tell you whether CBT is the right fit or whether another approach makes more sense.
Finding a CBT psychologist in Sydney
A few things worth knowing if you're looking:
Check AHPRA registration. All registered psychologists in Australia must be AHPRA-registered. Counsellors and therapists operate under different, less regulated frameworks.
Look for a clinical psychologist. Clinical psychologists have completed an additional two-year master's or doctoral programme specifically focused on the assessment and treatment of psychological disorders.
Consider telehealth. CBT translates extremely well online. If access or scheduling is a barrier, a telehealth session with an Australian-registered psychologist delivers the same treatment in a more flexible format.
If you're based in Sydney CBD and would like to explore whether CBT is right for you, I work with adults individually across anxiety, depression, OCD, trauma, insomnia, burnout, and men's mental health — in-person at my Elizabeth Street practice or via telehealth Australia-wide.
Book a session | Learn more about how therapy works
Alex Aslan is a registered psychologist (MClinPsych, Distinction) based in Sydney CBD, specialising in anxiety, trauma, men's mental health, and performance psychology.